
Mega Doctor News
Alzheimer’s disease, a type of dementia, is an irreversible, progressive brain disease that affects an estimated 5.7 million Americans. It is the sixth leading cause of death among all adults and the fifth leading cause for those aged 65 or older.
The causes of Alzheimer’s disease and other dementias are not completely understood, but researchers believe they include a combination of genetic, environmental, and lifestyle factors. In more than 90% of people with Alzheimer’s, symptoms do not appear until after age 60. The incidence of the disease increases with age and doubles every 5 years beyond age 65.
| Fast Facts |
| 15% of the US population is 65 or older. |
| Adjusting for age, rates of Alzheimer’s disease deaths increased more than 50%between 1999 and 2014. Alzheimer’s disease is the sixth leading cause of death among all US adults. |
| Americans fear losing their mental capabilities twice as much as they fear losing their physical abilities. |
| In 2018, total payments for health care, long-term care, and hospice for people with Alzheimer’s and other dementias are estimated to be $277 billion. |
| In 2018, more than 16 million Americans are providing more than 18.4 billion hours of unpaid care for family and friends with Alzheimer’s and other dementias. The total value of that care is over $232 billion. |
The Centers for Disease Control and Prevention (CDC) leads our nation’s public health efforts to help older adults with dementia to remain active, independent, and involved in their community by:
- Helping to promote awareness of Alzheimer’s disease and other dementias, including the importance of early diagnosis.
- Studying the societal and economic burden of dementias in states and communities.
- Supporting data collection on cognitive decline and caregiving.
- Working to ensure that caregivers have the resources to provide quality care to people with dementia.
Public Health Problem
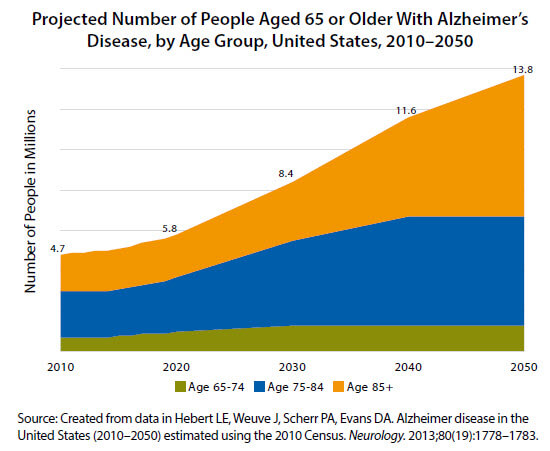
Alzheimer’s disease affects mainly older adults, and the growth in the number of older adults is unprecedented. In 2016, 49 million adults living in the United States—15% of the population—were 65 or older. By 2060, that number is expected to climb to about 95 million, or nearly 1 in 4 US residents. In 2018, total payments for health care, long-term care, and hospice for people with Alzheimer’s and other dementias are estimated to be $277 billion. Medicare pays almost half of these costs. Unless scientists discover how to prevent Alzheimer’s and other dementias, the number of people with these conditions, and the costs, will increase substantially.
Compromised Health and Quality of Life for Adults With Alzheimer’s Disease and Other Dementias
Alzheimer’s disease slowly destroys brain function, leading to cognitive decline (e.g., memory loss, language difficulty, poor executive function), behavioral and psychiatric disorders (e.g., depression, delusions, agitation), and declines in functional status (e.g., ability to engage in activities of daily living and self-care). People with Alzheimer’s gradually lose the ability to care for themselves and to remain independent. Twice as many Americans fear the loss of mental capabilities as the loss of physical ability.
Compromised Health and Quality of Life for Caregivers
Given longer life spans and the growing prevalence of conditions like Alzheimer’s, the need for caregivers, both informal (i.e., family and friends) and formal (i.e., paid professionals), will likely increase significantly as the US population ages. Although caregiving may be rewarding, caregivers are at an increased risk of increased stress, depression, unhealthy behaviors, and poor attention to their own health. Caregivers of people with dementias are at even higher risk of these problems, and they may delay their own health needs.
Informal or unpaid caregivers are the backbone of long-term care provided in people’s homes. According to 2009 data from the Behavioral Risk Factor Surveillance System (BRFSS), about 25% of US adults aged 18 or older reported providing care or assistance to a person with a long-term illness or disability in the past 30 days. In 2018, the value of this unpaid caregiver activity is an estimated $232 billion.
CDC’s Response
The National Center for Chronic Disease Prevention and Health Promotion (NCCDPHP) works in four key areas or domains: epidemiology and surveillance, environmental approaches, health care system interventions, and community programs linked to clinical services. This comprehensive approach supports healthy choices and behaviors, makes healthier options more available, and helps Americans better manage their health.
CDC works with partners—such as public health and aging services professionals, other federal agencies, universities, and community organizations—to improve the health of older adults.
With $4.5 million in FY 2018 funding, CDC’s Alzheimer’s Disease
and Healthy Aging Program supports these efforts by focusing its activities in two of NCCDPHP’s four domains: epidemiology and surveillance and community programs linked to clinical services.
Specifically, the program provides data and resources to practitioners in the areas of healthy aging and Alzheimer’s disease prevention and awareness, supports applied public health research, and helps national organizations share information and tools with the aging population.
Epidemiology and Surveillance
Collecting Data for Action: Cognitive Decline and Caregiving
CDC works with partners and states to gather information on the prevalence of cognitive decline and caregiving among adults, through BRFSS surveys. In 2015 and 2016, a total of 51 states and territories
Healthy Brain Research Network
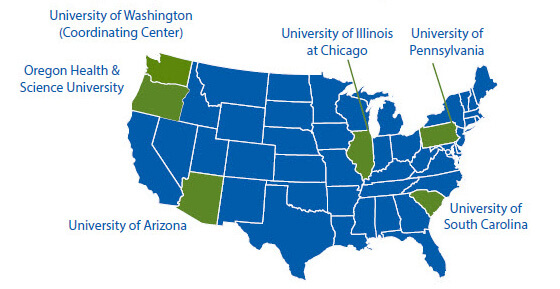
The Healthy Brain Research Network, a thematic network of CDC’s Prevention Research Centers Program, was started in 2014 to train future professionals and study cognitive health. These efforts support implementation of the Road Map.
added BRFSS questions about subjective cognitive decline to their surveys, and a total of 40 states and territories added questions about caregiving. States use this information to develop state plans, increase awareness about the needs of these populations, and guide elder justice and emergency preparedness efforts for older adults. State activities have resulted in the following accomplishments:
- Missouri used cognitive decline and caregiver data to help build the Seniors Count campaign to increase local services for seniors. The state also used the data in presentations to local public health agencies, webinars for state employees and public health staff, and other educational programs to improve awareness and early detection of cognitive decline.
- Louisiana used cognitive decline data to discuss Alzheimer’s and related dementias with insurers.
- Oregon used cognitive decline and caregiver data to get dementia included as a topic for Oregon’s Healthy Aging Summit, a part of the state’s Healthy Aging Initiative.
- Hawaii used cognitive decline data to develop Hawaii 2025: State Plan on Alzheimer’s Disease & Related Dementias.
Tracking Progress on Healthy People 2030
CDC co-chairs the Healthy People 2030 topic area and objectives on Dementias, Including Alzheimer’s Disease and has worked with several researchers to collect and analyze data for these objectives, which include increasing diagnosis and awareness and reducing preventable hospitalizations. CDC’s Alzheimer’s Disease and Healthy Aging Program and National Center for Health Statistics worked with the National Institute on Aging to add cognitive health measures to the baseline information collected for Healthy People 2030.
Community Programs Linked to Clinical Services
REACH OUT to Caregivers
REACH OUT is a training intervention for caregivers of people with Alzheimer’s disease or dementia. Caregivers who participated in REACH OUT had improved health and less depression after the training. The people they cared for were less likely to be left unsupervised, wander, or have access to dangerous objects.
Implementing a Community-Based Program for Dementia Caregivers: An Action Guide using REACH OUT expands REACH OUT’s effectiveness by providing examples, tips, resources, websites, and references to help communities use the intervention. This guide offers a step-by-step process for implementing REACH OUT in different kinds
of communities without losing the integrity of its design. Much of what appears in the guide can be applied to other evidence-based programs and is intended to expand interventions for caregivers and promote their adoption into widespread practice.












